Education
Pressure ulcers are a type of injury that breaks down the skin and underlying tissue. They are caused when an area of skin is placed under pressure. Also known as 'bedsores' or 'pressure sores,' Pressure ulcers can range in severity from patches of discoloured skin to open wounds that expose the underlying bone or muscle.
Pressure ulcers can develop when a large amount of pressure is applied to an area of skin over a short period of time. Or, when less pressure is applied over a longer period of time. The extra pressure disrupts the flow of blood through the skin. Without a blood supply, the affected skin becomes starved of oxygen and nutrients and begins to break down, leading to an ulcer forming. Pressure ulcers tend to affect people with health conditions that make it difficult to move, especially those confined to lying in a bed or sitting for prolonged periods of time.
There are two main goals when caring for people who are at risk of developing pressure ulcers. These are:
- to attempt to prevent the development of pressure ulcers by using special dressings and equipment, and by regularly changing a patient's position (to take pressure of different parts of the body at different times), and
- to treat existing pressure sores by cleaning them and by using antibiotics, improved nutrition and, in the most severe cases, surgery.
Where can Pressure Ulcers develop?
In short Pressure Ulcers can develop anywhere on the body however, areas of the body that are not protected by fat are most vulnerable.
- your shoulders, or shoulder blades
- your elbows
- the back of your head
- the rims of your ears
- your knees, ankles, heels, or toes
- your lower back, or hipbone
- the genitals (in men), and
- the breasts (in women)
Grading of pressure ulcers
There are four recognised grades of pressure ulcers in the EPUAP (European Pressure Ulcer Advisory Panel) Wound Classification system (visual references alongside).
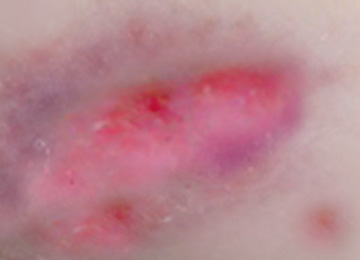
Grade 1:
Discolouration of intact skin not affected by light finger pressure (non blanching erythema).
This may be difficult to identify in darkly pigmented skin.
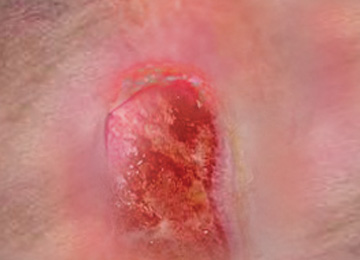
Grade 2:
Partial-thickness skin loss or damage involving epidermis and/or dermis.
The pressure ulcer is superficial and presents clinically as an abrasion, blister or shallow crater.
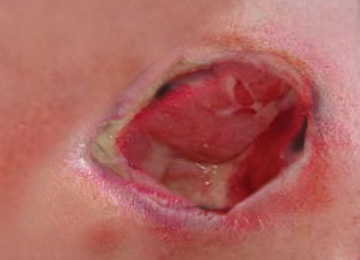
Grade 3:
Full thickness skin loss involving damage of subcutaneous tissue but not extending to the underlying fascia.
The pressure ulcer presents clinically as a deep crater with or without undermining of adjacent tissue.
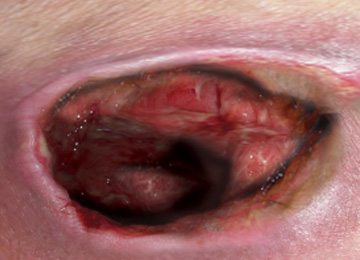
Grade 4:
Full thickness skin loss with extensive destruction and necrosis extending to underlying tissue.











